GASTROSCOPY
|
What is a gastroscopy?
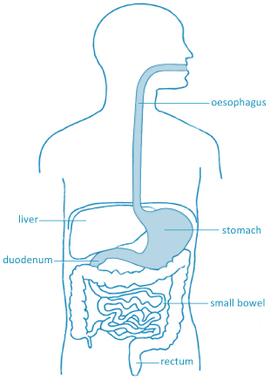
Also described as an ‘Upper GI endoscopy’, a gastroscopy is a procedure performed by an expert gastroenterologist to diagnose and in some cases, treat problems of the upper digestive system using an endoscope. An endoscope is a long thin flexible tube with a tiny video camera and a light on the end. By adjusting the various controls on the endoscope, your specialist can safely guide the instrument to carefully examine your oesophagus, stomach and duodenum, (the beginning of the small intestine). Most procedures are for diagnostic purposes, and may include the taking of biopsies (tissue samples) from the inner lining for examination by a pathologist. Sometimes the procedure is used for dilating (stretching) a narrowed portion of the oesophagus, or for the removal of polyps (abnormal growths) found during the examination. |
Is there an alternative to having a gastroscopy?
Depending on the reason your doctor has suggested a gastroscopy, there may be alternative tests available.
You can discuss these options with your doctor. Alternatives may include:
• CT scan – this special type of X-ray imaging produces images of the inside of your body.
No tissue biopsy is taken during this procedure.
• Ultrasound – this is another way to produce images of the inside of your body using
high-frequency sound waves. Again, no tissue biopsy is taken during this procedure.
• Barium meal – for this procedure, you drink a fluid that will show up on X-rays.
X-rays taken will show the inside of your oesophagus, stomach and duodenum.
How do I prepare for the procedure?
Please read and follow our Gastroscopy Preparation Instructions very carefully (these will be sent to you when you book in for your procedure. This will ensure your stomach is empty and that good views can be obtained during the procedure. You should have nothing to eat for 6 hours prior to the procedure (you can consume clear fluids until 3 hours prior to your procedure).
What do I do with my usual medications prior to the procedure?
• If you take warfarin, Plavix, Iscover, Pradaxa, or Insulin please contact Dr Halliday's rooms at least 7 days prior to the gastroscopy.
• Other medications are usually continued unless your doctor tells you not to. On the day of your procedure, you can take your regular
medications with a sip of water
What do I need to bring on the day of my procedure?
Please bring your doctor’s referral letter if available, health fund details and Medicare card. Please wear loose fitting clothing that can
be easily removed, as you may need to change into a patient gown. Any jewellery and valuables should be left at home.
What happens when I arrive at hospital?
You will be asked some basic questions about your health and medications. It is important to inform the staff if you have any dental crowns, bridges or loose teeth. If you wear dentures, you will be asked to remove them before the procedure. You will also be asked to remove any glasses, contact lenses or jewellery that you may be wearing. These will all be kept safe for you until after the procedure. If you have not
already done so, you will be asked to sign a form to verify your consent for the procedure and understanding of what is involved.
What will happen during the procedure?
During the procedure, every effort will be made to ensure you are as comfortable as possible. The anaesthetic doctor may spray the back of your throat with local anaesthetic to make the area go numb. A cannula (small needle) will be placed into the back of your hand through which sedative medication will be given. An oxygen mask will be put on and a blood pressure cuff placed on your arm. You will be asked to lie on your side on the hospital bed and a mouth guard placed over your teeth before the anaesthetic doctor gives you sedation. The sedative medication will put you into a deep sleep so that you will be comfortable during the procedure.
The endoscope will then be guided carefully through your mouth, into your stomach and duodenum (small bowel). Air is pumped through the endoscope to make the stomach expand so that it is easier to visualise. If necessary, biopsies and/or polyps will be taken/removed – this does not cause any pain. You will be in the treatment room for about 15-20 minutes.
What will happen after the gastroscopy?
Dr Halliday will speak with you before you go home. If any biopsies are taken, the results for these will take several days to be processed
and an arrangement for follow-up of these results will be made with you.
You must not drive, drink alcohol, sign legal documents or operate machinery for the first 24 hours after your procedure.
This is due to the sedative medication which may affect your concentration or co-ordination.
When can I go home?
You will be ready to go home approximately 2 hours after the procedure, however you must have someone to drive you home.
We also advise that you arrange for someone to stay with you for the first 24 hours.
Most patients do not have any problems after the procedure; but if you develop severe abdominal pain, fevers or chills, vomit blood, have difficulty breathing or any other symptoms that you are concerned about, you should contact your doctor (or the closest emergency department).
What are the risks of having a gastroscopy?
Gastroscopy is a common procedure that is generally safe and very well tolerated.
Common temporary side-effects include:
• Mild bloating – due to the air that was introduced to examine the stomach.
• Feeling sleepy or nauseated – due to the sedating medication
• A sore throat – due to the passage of the endoscope (lasting a few hours).
Gargling salt water or sucking throat lozenges will help ease this discomfort.
Complications are very rare, but may include:
• Perforation (a hole in the stomach or bowel wall) that may require surgery.
• Aspiration – If your stomach is not empty, occasionally you can vomit and aspirate stomach contents into your lungs.
This can cause pneumonia and require hospitalisation, oxygen and antibiotics.
• Bleeding – if biopsies are taken bleeding may occur causing you to vomit blood or pass black stools.
Very rarely, this may be severe enough to require hospitalisation, blood transfusions, a repeat gastroscopy or even open surgery.
• Tooth damage/ cut lip – a protective mouthguard is used to reduce your risk.
• Death is extremely rare, although this is a possible consequence of any medical procedure.
• Failed procedure - occasionally a gastroscopy may not be successfully completed and need to be repeated at a later date.
If you wish to discuss the details of all possible rare complications, you should inform your doctor and/or anaesthetist prior to the procedure.
Exact risks will differ for every person – so ask your doctor how these risks apply to you.
Depending on the reason your doctor has suggested a gastroscopy, there may be alternative tests available.
You can discuss these options with your doctor. Alternatives may include:
• CT scan – this special type of X-ray imaging produces images of the inside of your body.
No tissue biopsy is taken during this procedure.
• Ultrasound – this is another way to produce images of the inside of your body using
high-frequency sound waves. Again, no tissue biopsy is taken during this procedure.
• Barium meal – for this procedure, you drink a fluid that will show up on X-rays.
X-rays taken will show the inside of your oesophagus, stomach and duodenum.
How do I prepare for the procedure?
Please read and follow our Gastroscopy Preparation Instructions very carefully (these will be sent to you when you book in for your procedure. This will ensure your stomach is empty and that good views can be obtained during the procedure. You should have nothing to eat for 6 hours prior to the procedure (you can consume clear fluids until 3 hours prior to your procedure).
What do I do with my usual medications prior to the procedure?
• If you take warfarin, Plavix, Iscover, Pradaxa, or Insulin please contact Dr Halliday's rooms at least 7 days prior to the gastroscopy.
• Other medications are usually continued unless your doctor tells you not to. On the day of your procedure, you can take your regular
medications with a sip of water
What do I need to bring on the day of my procedure?
Please bring your doctor’s referral letter if available, health fund details and Medicare card. Please wear loose fitting clothing that can
be easily removed, as you may need to change into a patient gown. Any jewellery and valuables should be left at home.
What happens when I arrive at hospital?
You will be asked some basic questions about your health and medications. It is important to inform the staff if you have any dental crowns, bridges or loose teeth. If you wear dentures, you will be asked to remove them before the procedure. You will also be asked to remove any glasses, contact lenses or jewellery that you may be wearing. These will all be kept safe for you until after the procedure. If you have not
already done so, you will be asked to sign a form to verify your consent for the procedure and understanding of what is involved.
What will happen during the procedure?
During the procedure, every effort will be made to ensure you are as comfortable as possible. The anaesthetic doctor may spray the back of your throat with local anaesthetic to make the area go numb. A cannula (small needle) will be placed into the back of your hand through which sedative medication will be given. An oxygen mask will be put on and a blood pressure cuff placed on your arm. You will be asked to lie on your side on the hospital bed and a mouth guard placed over your teeth before the anaesthetic doctor gives you sedation. The sedative medication will put you into a deep sleep so that you will be comfortable during the procedure.
The endoscope will then be guided carefully through your mouth, into your stomach and duodenum (small bowel). Air is pumped through the endoscope to make the stomach expand so that it is easier to visualise. If necessary, biopsies and/or polyps will be taken/removed – this does not cause any pain. You will be in the treatment room for about 15-20 minutes.
What will happen after the gastroscopy?
Dr Halliday will speak with you before you go home. If any biopsies are taken, the results for these will take several days to be processed
and an arrangement for follow-up of these results will be made with you.
You must not drive, drink alcohol, sign legal documents or operate machinery for the first 24 hours after your procedure.
This is due to the sedative medication which may affect your concentration or co-ordination.
When can I go home?
You will be ready to go home approximately 2 hours after the procedure, however you must have someone to drive you home.
We also advise that you arrange for someone to stay with you for the first 24 hours.
Most patients do not have any problems after the procedure; but if you develop severe abdominal pain, fevers or chills, vomit blood, have difficulty breathing or any other symptoms that you are concerned about, you should contact your doctor (or the closest emergency department).
What are the risks of having a gastroscopy?
Gastroscopy is a common procedure that is generally safe and very well tolerated.
Common temporary side-effects include:
• Mild bloating – due to the air that was introduced to examine the stomach.
• Feeling sleepy or nauseated – due to the sedating medication
• A sore throat – due to the passage of the endoscope (lasting a few hours).
Gargling salt water or sucking throat lozenges will help ease this discomfort.
Complications are very rare, but may include:
• Perforation (a hole in the stomach or bowel wall) that may require surgery.
• Aspiration – If your stomach is not empty, occasionally you can vomit and aspirate stomach contents into your lungs.
This can cause pneumonia and require hospitalisation, oxygen and antibiotics.
• Bleeding – if biopsies are taken bleeding may occur causing you to vomit blood or pass black stools.
Very rarely, this may be severe enough to require hospitalisation, blood transfusions, a repeat gastroscopy or even open surgery.
• Tooth damage/ cut lip – a protective mouthguard is used to reduce your risk.
• Death is extremely rare, although this is a possible consequence of any medical procedure.
• Failed procedure - occasionally a gastroscopy may not be successfully completed and need to be repeated at a later date.
If you wish to discuss the details of all possible rare complications, you should inform your doctor and/or anaesthetist prior to the procedure.
Exact risks will differ for every person – so ask your doctor how these risks apply to you.